You ever wake up after a long flight and think your feet belong to a cartoon character? Like, seriously, they’re all puffy and swollen. That’s edema for ya!
So what is it, anyway? Well, it’s when your body decides to hold onto too much fluid. And trust me, it can happen for a bunch of reasons.
You could be sitting too long, eating salty snacks like there’s no tomorrow, or even just running a marathon (which sounds exhausting). Your body’s just acting like that friend who can’t let go of the party snacks.
But here’s the kicker: edema isn’t just about bloated ankles or puffy eyes. There’s some real science simmering underneath all that swelling. It’s like your body’s way of sending up a flare saying, “Hey! Something’s off here!” So grab a comfy seat, and let’s unpack this fascinating phenomenon together!
Understanding Edema: The Scientific Mechanisms and Causes Behind Fluid Retention in the Body
So, let’s talk about edema. It’s a fancy term for when your body holds onto too much fluid, usually in your legs, feet, or even your hands. It can happen to any of us at some point. I remember a time after a long flight; my feet looked like balloons! It was uncomfortable and annoying.
Now, what causes this situation? Well, edema can spring from various factors. Generally, it occurs when there’s an imbalance in how fluids move within your body. Picture it as a tug-of-war between the blood vessels and the surrounding tissues.
- Blood Pressure: When your blood pressure is high, it can push more fluid out of your blood vessels and into the surrounding tissues.
- Sodium Intake: Eating salty foods makes you retain water. You know that bloated feeling after a pizza? That’s sodium at work!
- Gravity: Standing or sitting for too long causes fluid to settle in your lower extremities. That’s why you might notice swollen ankles after a day on your feet.
- Injury or Infection: If you’ve ever sprained an ankle, you’d have seen swelling around the area. That’s edema in action as your body sends extra fluid to help with healing.
- Meds: Some medications can also cause retention as a side effect. For instance, certain blood pressure medicines can mess with how fluids balance out.
- Heart or Kidney Problems: If your heart isn’t pumping effectively or if kidneys aren’t filtering well, it can lead to more serious cases of edema.
The thing is, our bodies are pretty good at balancing liquids most of the time. There are tiny capillaries that help manage fluid distribution. They have tiny pores that open and close depending on various signals from hormones and other chemicals in our system.
Beneath all this is something called oncotic pressure. It pulls fluid back into blood vessels thanks to proteins like albumin. If you have low levels of these proteins—say due to liver disease—you might find yourself dealing with more edema than usual.
A lot of people think swelling is just harmless water retention which isn’t always the case! Sometimes it signals underlying health issues that need attention. So keep an eye on those symptoms! And remember: if you’re dealing with persistent swelling or pain, it’s best to chat with a healthcare professional.
If you’re ever sitting there struggling with swollen feet after indulging in that massive steak dinner or long flight, just remember—your body has its reasons for acting that way. Fluid retention might be annoying but understanding what’s behind it helps make sense of our mysterious bodies!
The Science Behind Swelling: Understanding Inflammation in Biological Systems
Swelling, or inflammation, is something most of us have experienced at some point. You know that feeling when you twist your ankle and it balloons up like a balloon animal? Yeah, that’s inflammation at work! Basically, it’s your body’s way of reacting to injury or infection. Let’s break this down.
When an injury happens—like smashing your toe against the coffee table—tiny blood vessels in the area get damaged. This leads to a chain reaction. First off, blood flow increases to the area. That’s why you see redness and feel warmth; more blood means more healing resources flowing in.
To help understand swelling better, think about this:
- The Body’s Defense Mechanism: Inflammation is part of your immune response. It’s like calling in reinforcements when there’s trouble. The immune cells come charging in to tackle any foreign invaders and start the healing process.
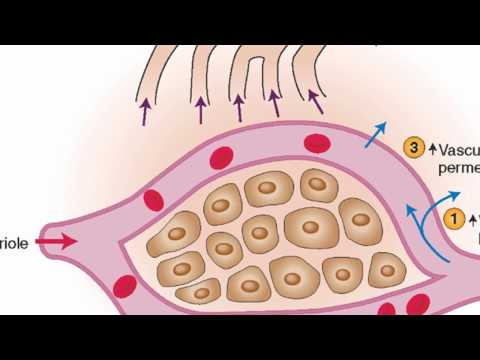
- The Chemicals Involved: Your body releases various substances like histamines and prostaglandins that make blood vessels leakier. This allows more fluid and white blood cells to escape into the tissues where they’re needed most.
- The Resulting Edema: The build-up of these fluids leads to what we call edema—where body parts swell up due to excess fluid accumulation.
This whole process can be thought of as a well-orchestrated team effort involving different players: immune cells, chemical signals, and blood vessels all working together. But what if inflammation goes haywire? Sometimes it can stick around longer than needed or happen when it’s not even necessary—like with allergies or chronic diseases like arthritis.
A neat little example is rheumatoid arthritis. Here, your immune system decides to wage war on your own joints! This results in long-term inflammation—when you touch those joints, they might feel warm and swollen, just like a bruised finger after stubbing it.
So why does this actually matter? Because understanding swelling helps medical folks figure out how best to treat injuries. If you know that inflammation can be both good (to help heal) and bad (when it sticks around), doctors can target their treatments better—you follow me?
To wrap this up: swelling isn’t just about being uncomfortable; it’s a sign that your body is kicking into action! Just keep in mind that while some inflammation is helpful for healing, too much or prolonged inflammation can lead to problems down the road. It’s like a dance between protection and healing versus potential harm!
Comprehensive Guide to the Pathophysiology of Edema: Downloadable PDF Resource for Medical Science
Edema, huh? It’s that swelling you often see in feet or hands, and it can be super annoying. But what’s really going on under the surface? There’s a lot to unpack in the pathophysiology of edema.
First off, it helps to understand that edema happens when fluid builds up in the tissues. This can be due to various reasons; most commonly, it comes from issues with blood vessels, lymphatic systems, or even certain organs like your heart or kidneys.
So why does this fluid get stuck? Well, there are a few mechanisms at play here:
- Increased Hydrostatic Pressure: This is like when you’re trying to squeeze too much into a balloon and it starts bulging out. If there’s increased pressure inside your blood vessels—maybe due to heart failure—it forces fluid out into surrounding tissues.
- Decreased Oncotic Pressure: Imagine a sponge that’s supposed to soak up water but can’t because it’s damaged. Proteins in your blood like albumin normally help draw fluid back into capillaries. If you’ve got low protein levels (like from liver disease), fluid spills out.
- Lymphatic Obstruction: Your lymphatic system is kind of like a drainage system for excess fluids. If it’s blocked—because of surgery, infection, or other reasons—fluid can’t drain away properly.
Okay, now picture this: You had a long day at work and your feet are killing you by the time you get home. Your body’s been working hard all day, pumping blood around and dealing with gravity pulling things downwards. That extra pressure can lead to pooling of fluid in your lower extremities—classic edema.
Types of edema are also worth noting:
- Pitting Edema: Press on the swollen area with your finger and see a dent left behind? That’s pitting edemas telling you there’s some serious fluid accumulation.
- Non-Pitting Edema: Here, nothing changes when you press down. Might indicate conditions like lymphedema or thyroid problems.
And there’s more! Systemic conditions could lead to edema too—think kidney disease causing the body to retain sodium and water because it can’t filter properly.
Okay, so where’s this all leading? Understanding these mechanisms helps medical professionals figure out how best to treat edema based on its cause. They might recommend medications to lower blood pressure or improve heart function if that’s the issue.
That trip down edema lane shows how interconnected our body systems are! It’s fascinating yet complex stuff that reminds us how important balance is.
So next time you see someone with swollen legs or feel it yourself after a long day standing around—just remember: there’s quite a scientific story behind those bulges!
You know that feeling when your feet get all puffy after a long day? It’s like they’ve turned into marshmallows or something. Well, that’s edema for you! It happens when your body retains too much fluid, and it can pop up in various parts, like your legs, ankles, or even your hands. Let’s take a peek behind the scenes at what’s going on.
Edema is really all about fluid balance. There’s this fancy term called “homeostasis.” Basically, it means your body likes to keep things balanced. Fluids move in and out of blood vessels all the time. This movement is regulated by a couple of key players: blood pressure and the proteins in your blood.
When blood pressure gets high—maybe because you’ve been running around too much or even from eating too much salt—more fluid leaks out of the vessels into surrounding tissues. It’s like if you had a balloon full of water; if you keep poking it with a pin, water starts seeping out everywhere!
And then there are those proteins, especially albumin. Albumin helps keep fluid inside your blood vessels. If something goes wrong and those protein levels drop (which can happen for various reasons), suddenly there’s less “glue” holding the fluids in check. Boom! Edema strikes.
I remember once after hiking all day—I was so pumped about the views and forgot to drink enough water—but my feet felt ridiculously swollen by the end of it! That was my body trying to cope with dehydration while also retaining more water to make up for it. Talk about an unexpected twist on a fun adventure!
Now, there are other things at play too—like inflammation or heart problems—that can also lead to edema. When tissues get inflamed, they become leaky and allow extra fluid to sneak through those blood vessel walls, which just adds to the puffiness.
So next time you notice some swelling or puffiness somewhere on your body, remember what’s happening beneath the surface: It’s not just random; there are these complex little battles going on with fluids and proteins trying to maintain balance in our incredible bodies! It’s kind of amazing how everything is connected and how much our bodies work behind the scenes without us even realizing it!