So, picture this: you’re at a party, right? Everyone’s chatting about the latest movie or that new viral dance challenge. But then, someone starts talking about osteochondromatosis. Yeah, I know! Not exactly the hottest topic at a shindig. But here’s the thing—this condition is super interesting if you dig into it a bit.
Imagine tiny bony growths popping up where they shouldn’t be—like an unexpected guest showing up at your place. Seriously, you can almost hear the bones whispering “What are we doing here?” This condition isn’t just a quirky medical curiosity; it can seriously impact folks’ lives.
In this little dive into radiology insights, we’re gonna unpack what osteochondromatosis really means for clinicians and researchers alike. It’s not all doom and gloom! Trust me, understanding these bony party crashers can really help in diagnosis and treatment planning. So pull up a chair and let’s sort through this together!
Advanced Insights into Synovial Chondromatosis: Radiological Diagnosis and Imaging Techniques
Alright, let’s get into the nitty-gritty of synovial chondromatosis and how radiological diagnosis and imaging techniques play a key role. It’s one of those conditions that can seem pretty complex at first, but once you break it down, it all starts to make sense.
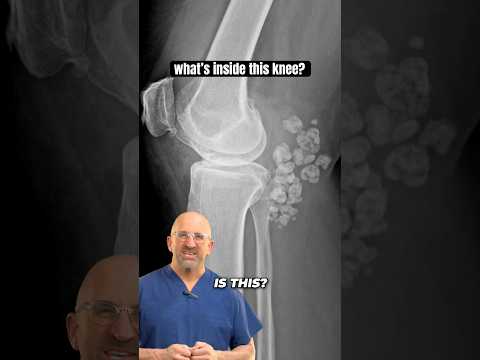
So, synovial chondromatosis is a rare condition where the synovium—the lining of your joints—starts to produce cartilage nodules. These nodules can become loose bodies in the joint space. Imagine little marbles floating around in there, causing all sorts of trouble! It most often affects the knee but can pop up in other joints, like the hip or elbow too.
For clinicians and researchers, diagnosing this condition quickly and accurately is crucial because it can lead to significant joint pain and dysfunction if left untreated. That’s where imaging techniques come into play.
When it comes to radiological diagnosis, there are a few main players:
- X-rays: These are usually the first step. They help you see any calcified loose bodies within the joint. You might notice some changes in bone structure too.
- MRI: This one is big because it provides detailed images of soft tissues. MRI shows us not just those pesky nodules but also whether there’s any surrounding inflammation or joint effusion.
- CT scans: Computerized tomography is super useful for a closer look at bone structures. It can reveal details about the size and shape of those cartilage nodules.
Imagine you’re figuring out why your dog won’t fetch anymore—it could be anything from a toy under the couch to something more serious like an injury. Each imaging technique gives you different clues about what might be going on with that joint.
Now here’s something really interesting: when looking at an MRI for synovial chondromatosis, you often see low-signal intensity on T1-weighted images and high-signal intensity on T2-weighted images for those cartilage nodules. It’s kind of like looking at shadows versus bright spots; they tell different stories about what’s happening inside.
What makes things trickier is differentiating synovial chondromatosis from other similar conditions like osteoarthritis or even pigmented villonodular synovitis (PVNS). You’ve got to pay attention to certain details on imaging—like the presence of multiple loose bodies or specific patterns in how they appear—to make an accurate diagnosis.
So yeah, it’s not just about spotting those little marbles; it’s about piecing together a puzzle based on various clues from different imaging techniques. And that’s crucial not only for treatment planning but also for patients’ quality of life.
Ultimately, understanding these insights into radiological diagnosis can help clinicians provide better care. The goal is to catch synovial chondromatosis early so that effective treatments can be initiated before things get too complicated—because who wants their joints feeling like they’re playing dodgeball with all those loose bodies?
Comparative Radiological Analysis of PVNS and Synovial Chondromatosis: Diagnostic Insights in Joint Pathologies
When it comes to joint issues, two conditions often pop up: Pigmented Villonodular Synovitis (PVNS) and Synovial Chondromatosis. Both can be a pain—literally! But they’ve got different characteristics that set them apart. Knowing the differences can really help with getting the right treatment and diagnosis.
Pvns is a rare joint disorder that usually affects the knee but can show up in other joints too. It’s kind of like an overgrowth of the tissue lining your joints, which leads to inflammation and sometimes pain or swelling. Remember that feeling of hitting your funny bone? Imagine that, but it sticks around longer because of the irritation from this tissue growth.
On the other hand, Synovial Chondromatosis involves the formation of cartilage nodules within the joint space. And while it sounds super serious, think of it more like an annoying buildup rather than just inflammation. These nodules can break loose and float around in the joint, causing all kinds of chaos when they get jammed in places they shouldn’t be.
- Affected population: PVNS usually strikes younger adults, while Synovial Chondromatosis tends to show up in middle-aged folks.
- Main symptoms: Both can lead to joint pain and swelling, but PVNS often comes with notable tenderness and a sense of warmth in the affected area.
- X-ray findings: This is where radiology really kicks in! In PVNS, you might see soft-tissue masses or erosion on X-rays. Synovial Chondromatosis will show those charming little nodules floating around—like tiny rocks!
Getting an accurate diagnosis is huge because treatments differ. For example, PVNS might require surgery to remove those pesky tissue overgrowths. Whereas with Synovial Chondromatosis, surgery could involve just removing those nodules without affecting surrounding tissues too much.
A personal experience here: My friend’s dad had something similar to these conditions. After months of nagging pain in his knee—like he’d run a marathon on a broken leg—he finally went for an MRI. Turns out he had weird floating cartilage bits causing all his trouble! It was eye-opening how something so small could disrupt daily life!
The takeaway? If you’re dealing with mysterious joint pains or have been given a diagnosis you’re not quite sure about, radiological analysis makes all the difference. With careful examination and understanding how these conditions manifest on images like X-rays or MRIs, clinicians can better tailor their approach for effective treatment!
You see? It’s always crucial to keep these distinctions clear in your head—even if it sounds complicated at first glance! Every little detail helps paint a better picture for the folks trying to help you feel better!
Sessile Osteochondroma: Advanced Radiological Insights and Diagnostic Approaches in Musculoskeletal Science
Let’s jump into the world of sessile osteochondromas! These little guys are actually pretty interesting when you think about it. They’re benign bone tumors that usually hang around near the growth plates of bones—especially in kids and young adults. So, if you’ve heard the term “osteochondromatosis,” you’re already in the right ballpark!
Sessile osteochondroma is like the more compact cousin of its pedunculated variant. While pedunculated ones have a stalk, sessile ones are directly attached to the bone without this feature. This means they can sometimes be a bit trickier to spot on X-rays or MRIs since they’re flat against the bone.
When it comes to imaging, there are several things you should keep in mind:
- X-rays: These are often the first tools used because they’re quick and easy. You may see a well-defined area that looks like a tiny bump on the bone. It’s important to note that these bumps can sometimes look similar to other conditions.
- CT scans: CTs can give a more detailed view of the bone structure, allowing for better assessment of whether there’s any cortical involvement. That means you can see if it’s affecting more than just the surface layer of bone.
- MRI: This is super handy for checking out soft tissue changes around these tumors, which can help identify any potential complications or adjacent issues like cartilage involvement.
One particularly tricky part? Sometimes sesile osteochondromas can be mistaken for malignant tumors if they’re not analyzed properly. Like I remember this one case—a kid came in with what seemed to be severe swelling around his knee, and everyone was worried about cancer. But after some careful imaging and analysis, turns out it was just this pesky osteochondroma.
You might wonder how doctors differentiate between these conditions. Well, one major clue involves looking at margins. A benign tumor usually has well-defined edges while something more serious tends to be irregular or fuzzy around its borders.
The process for diagnosing sessile osteochondromas doesn’t stop just at imaging either! Clinicians often rely on:
- Clinical examination: Looking for symptoms like pain or discomfort—is it caused by pressure from surrounding tissues? The history is also vital: has there been any trauma?
- Monitoring growth: If an osteochondroma is growing during adulthood, that could raise red flags that need further investigation.
- Biospy: Though not common for each case since they’re benign, sometimes a sample may be taken if there’s uncertainty about what you’re dealing with.
In terms of treatment options? Many times, no action is required unless there’s discomfort or complications like impingement or fractures due to size. But surgical removal can be suggested if needed.
So there you have it! Sessile osteochondromas might seem small but understanding them really takes a rounded approach—from radiological insights to hands-on diagnosis techniques! Always remember that accurate diagnosis is key because we want to avoid those “Oh no!” moments in clinical practice when something benign gets mistaken for something serious!
Osteochondromatosis, wow, that’s quite a mouthful, isn’t it? You probably won’t hear that on a first date or anything. But seriously, this is one of those conditions that can really mess with someone’s life if it’s not caught early enough. It’s often linked to the growth of benign tumors on bones and cartilage, specifically arising from the growth plate. Imagine walking around with these little bumpy surprises on your bones. Not fun!
So here’s the thing: radiology plays a super crucial role in diagnosing this condition. You see, when you get those X-rays or MRIs done, they reveal more than just bone structures; they show us clues about what’s going on underneath all that skin. For clinicians and researchers alike, interpreting these images is like piecing together a puzzle—one wrong piece and you could end up with a totally different picture.
As I think about it, I remember my friend Sarah who went through something similar. She had persistent knee pain for years and couldn’t figure out what was up. After countless visits to specialists and endless tests that felt like she was going through an obstacle course of healthcare, it finally turned out she had osteochondromatosis. The diagnosis opened doors for her treatment options but also made her reflect on how her body dealt with pain all this time.
In terms of radiology insights, there’s often this delicate balance between spotting those pesky lesions in their early stages and understanding their potential implications down the line. A key challenge for researchers is refining imaging techniques to see even the tiniest changes over time—something that can impact how soon someone starts treatment or even how they manage their symptoms.
It’s easy to overlook these details when you’re focused solely on treatment plans without considering how they connect with imaging results. And let’s face it; most of us aren’t fluent in radiology speak! But for doctors working with patients like Sarah—or even for researchers delving into the latest studies—having a deeper grasp of osteochondromatosis through imaging makes all the difference in figuring out the best way forward.
At the end of the day, we’re talking about people who have lives to live and dreams to chase! It’s fascinating how something so technical as radiology can have such personal impacts. So yeah, whether you’re scrolling through images or treating patients directly, remember: there’s always more than meets the eye—or should I say more than meets the X-ray?