You know that moment when you accidentally stand on a Lego? Yeah, instant pain, right? Well, imagine if that kind of pain was playing hide and seek in your body. Kinda wild to think about how our body works, isn’t it?
So here’s the deal. We’ve got this whole world inside us where things are constantly buzzing and changing. Cells chatting away, systems working overtime—like a backstage crew in a crazy show.
But sometimes, things go off script; cells get confused or rebel a bit. That’s where the fascinating mess of pathophysiology comes into play. It’s like trying to figure out why the pizza delivery is late when you’re starving!
In this little journey together, we’ll dig into what really happens when your body’s not playing nice. You ready? Let’s get into some juicy insights!
Understanding the Pathophysiology of Typical Hemolytic Uremic Syndrome: Insights from Clinical Science
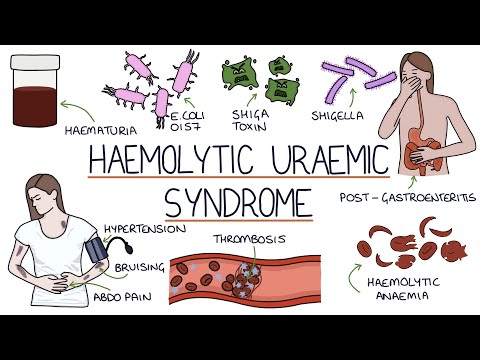
So, when we talk about Typical Hemolytic Uremic Syndrome (HUS), we’re diving into a pretty serious and complicated topic. You might be thinking, “What even is that?” Well, HUS is primarily a condition that can occur after an infection, usually caused by a type of bacteria called Escherichia coli, or E. coli for short. This particular bug produces toxins that can wreak havoc on the body.
The first thing to understand is how this whole process kicks off. After you ingest contaminated food or water, the E. coli bacteria start to multiply in your intestines. They then release toxins known as Shiga toxin. This toxin enters your bloodstream and can start causing real trouble, leading to hemolysis—basically the destruction of red blood cells.
This destruction happens because the Shiga toxin damages the endothelial cells lining your blood vessels. These cells are like tiny gates controlling what can pass through into tissues. Once they’re hurt, they stop functioning right and can lead to clots forming in small blood vessels—a condition known as thrombotic microangiopathy.
- First up, you get hemolytic anemia, which is when you have fewer red blood cells to carry oxygen around your body.
- This is often followed by thrombocytopenia, where there are fewer platelets available for clotting—yeah, not good at all.
- The last punch comes from kidney injury because those tiny clots block blood flow there too.
Your kidneys might end up swelling and losing their ability to filter waste from your bloodstream correctly. Can you imagine all those toxins just piling up? Yikes! This kidney damage can sometimes lead to complete kidney failure if not treated properly.
A quick story: I once heard about a family picnic gone wrong when everyone ate undercooked hamburgers. A couple of kids ended up getting sick—one of them had HUS after being infected with E. coli from those burgers! It’s one of those painful reminders that food safety really matters!
Treatment for HUS typically involves supportive care. This could mean hydration, managing electrolyte imbalances, and sometimes dialysis if the kidneys aren’t working well enough. Doctors might also monitor for complications since HUS can play out differently in each person.
The key takeaway here is that while HUS often follows an infection with E. coli, its effects resonate through our bodies in several harmful ways—hemolysis, thrombocytopenia, and kidney damage all playing their parts in this disturbing play.
So now when someone mentions Typical Hemolytic Uremic Syndrome, you’ve got a sense of what’s going on behind the scenes! Seriously fascinating stuff when you think about how our bodies react to these tiny invaders!
Understanding the Pathophysiology of Hemolytic Uremic Syndrome: Insights into Mechanisms and Implications in Clinical Science
Alright, let’s break down Hemolytic Uremic Syndrome (HUS) and its pathophysiology in a way that makes sense, you know?
Hemolytic Uremic Syndrome is an illness that mainly affects the kidneys but involves other parts of the body too. It often happens after a severe infection, most commonly due to a specific strain of bacteria called Escherichia coli, or E. coli. You might have heard of this because it can cause food poisoning.
Now, when this bacteria gets into your system, it produces toxins that can lead to some pretty serious problems. The main toxin involved is called Shiga toxin. This is where things get tricky. The toxin damages the blood vessels in your body and especially targets the kidneys.
Once the blood vessels are damaged, there are several things going on that lead to HUS:
- Hemolysis: This is a fancy word for the destruction of red blood cells. The damaged vessels cause them to break apart too early.
- Thrombocytopenia: This means you have low platelet levels. Platelets help with clotting, and when you don’t have enough, you can bleed easily.
- Acute Kidney Injury: With all this chaos happening in your blood vessels, your kidneys start to take a hit. They can’t filter waste properly anymore.
So why does all this matter? Well, when someone develops HUS, they might experience symptoms like diarrhea (often bloody), fatigue from anemia, and decreased urination because their kidneys aren’t working right. It’s pretty scary stuff!
Not only is HUS diagnosed based on symptoms but also through lab tests looking for signs of hemolysis or kidney dysfunction. Here’s where clinical science steps in: understanding these mechanisms helps doctors figure out how best to treat patients.
One common treatment approach might include giving patients fluids and electrolytes to maintain hydration and support kidney function. Sometimes they even need dialysis if their kidneys are really struggling.
The journey doesn’t stop at treatment; there’s ongoing research into how we can better understand HUS and its long-term effects on health. For example, children who recover from HUS could face complications later on; monitoring them becomes crucial.
You see? The pathophysiology of HUS isn’t just a bunch of medical jargon; it represents real lives affected by this condition. When we grasp these underlying mechanisms, we make steps toward improving care for those impacted by this syndrome!
Essential Insights into Hemolytic Uremic Syndrome: Key Concepts for Students in Science Education
Hemolytic Uremic Syndrome (HUS) is a serious condition, and understanding its pathophysiology is crucial for students in science education. So, what exactly happens in HUS? Let’s break it down.
Basically, HUS is often triggered by an infection caused by Escherichia coli, specifically the strain called E. coli O157:H7. This bacterium usually comes from undercooked meat or contaminated food and can lead to quite a nasty case of diarrhea—sometimes bloody.
Now, here’s where it gets interesting. After the initial infection, these bacteria produce toxins that damage cells in the blood vessels. This can lead to a cascade of issues:
- Red Blood Cell Destruction: The toxins damage red blood cells, which can cause anemia.
- Kidney Damage: The kidneys filter blood and clear toxins from the body. Damage from toxins leads to acute kidney injury, which is a hallmark of HUS.
- Platelet Activation: The condition also causes unusually high platelet activity. When platelets are activated excessively, it can lead to small clots forming throughout the body.
The combination of these factors causes decreased blood flow to various organs and can result in serious complications. I remember a friend who got sick after eating at a barbecue place; within days he was in the hospital because his kidneys took a hit from HUS—definitely not the way you want your summer cookouts to end!
Treatment for HUS primarily focuses on managing symptoms and preventing complications. This often includes supportive care like fluids for hydration and sometimes dialysis if the kidneys aren’t working at all. It’s amazing how this condition really emphasizes how interconnected our systems are. It’s like one little bacterial infection can spiral into something that affects multiple organs!
If you’re diving into this topic as part of your studies, keep an eye out for research on potential prevention strategies too! With better food safety guidelines and awareness about proper cooking practices, we could reduce cases of HUS significantly.
The key takeaway here? Understanding HUS helps us appreciate not just human health but also how infections can severely impact our bodies’ functions. And that knowledge is super important as you continue your journey in science education.
You know, when you think about diseases, it’s easy to get lost in all the medical jargon. Like, what even is pathophysiology? Sounds fancy, right? Well, it’s really just about understanding how diseases affect the body—what goes wrong and why. And that’s where insights from hus pathophysiology come into play.
I remember sitting in class one day, surrounded by textbooks filled with complicated diagrams and dense paragraphs. My professor was explaining how specific conditions could disrupt our normal bodily functions. At first, my eyes glazed over; it felt so distant. But then she shared a story about a patient struggling with a rare genetic disorder. The way her face lit up while discussing that person’s journey really struck me. It wasn’t just information anymore; it was human.
So when we talk about hus pathophysiology—specifically in conditions like Huntington’s disease—you see a vivid picture emerge. You’ve got this genetic mutation leading to neurodegeneration. Basically, certain brain cells start to die off over time. This means loss of movement control, cognitive decline—the whole package that dramatically affects someone’s life and their loved ones’ lives too.
But here’s the kicker: if we can break this complex stuff down into relatable stories—like the one I heard in class—it becomes easier for everyone to understand. It’s not just some textbook stuff anymore; it’s something that impacts real lives! Sharing these insights means we aren’t just teaching; we’re connecting people to science in a way that feels tangible.
Plus, this knowledge can inspire conversations around research funding or community support for those affected by these conditions. When you grasp the deeper meaning behind what happens at the cellular level during a disease process like Huntington’s disease, you start to realize there’s hope for treatment and better quality of life.
And honestly, that’s something worth sharing with others—making science accessible and showing how it relates back to our everyday experiences makes all of this feel real. After all, isn’t that what scientific outreach is about? Connecting stories with science so people can truly get involved and maybe even spark some change?