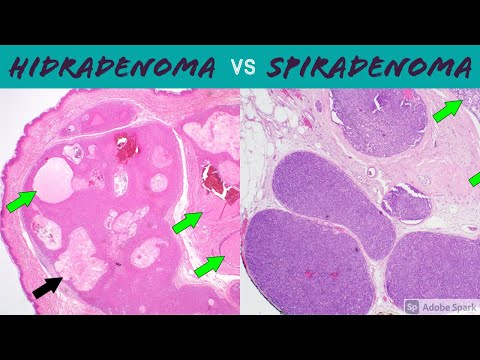
So, picture this: you’re hanging out with your friend, and they casually mention having this weird little bump under their skin. You’re like, “Whoa, what’s that?” Turns out it’s a hidradenoma. I mean, sounds kind of fancy and scary, right?
Well, the thing is, these little bumps are way more common than you might think. They can pop up in some pretty unexpected places! But what are they really? And why should we care about them?
Let’s break it down together. Seriously, once you peel back the layers, there’s a ton of interesting stuff about how these things form and what they can mean for our health. So grab a snack and let’s dig into this relatively unknown world of hidradenoma!
Hidradenoma Pathology: Comprehensive Outlines and Insights for Scientific Research
So, let’s chat about hidradenoma pathology. You might be thinking, what in the world is that? Well, hidradenomas are these benign tumors that pop up in the sweat glands of your skin. It’s like having an unwanted guest that doesn’t really do anything harmful but just hangs around.
These tumors primarily arise from the **apocrine sweat glands**, which are found mainly in areas like your armpits and groin. They can also surface where sebaceous glands are present. Imagine disturbing a cozy neighborhood of glands—yeah, that’s sort of what’s happening here.
Clinical Significance: Alright, so why should we care about these little guys? Even though they’re benign—meaning not cancerous—they can cause some issues, like skin irritation or cosmetic concerns for those who have them. Plus, it’s essential to distinguish them from malignant tumors to avoid unnecessary stress or treatment. You know how some things just can’t be left alone because they look suspicious?
Now let’s break down a few key points about hidradenomas:
- Types: There are several types of hidradenomas, with **syringomatous** and **clear cell** being the most common ones you’ll hear about.
- Symptoms: Usually, they present as painless bumps on the skin. They might feel firm and could vary in size.
- Diagnosis: A proper diagnosis usually involves a physical exam and may require a biopsy to confirm they’re not malicious.
- Treatment: Most people opt for surgical removal if it becomes bothersome or for cosmetic reasons. It’s like tidying up your living room; sometimes you just need to clear out stuff!
In terms of research insights, scientists are still digging deep into understanding how these things develop—like what genetic markers might be involved or if they’re linked to other conditions. Some studies suggest certain mutations play a role in their formation.
There was this one time when I saw an intern dealing with a case of hidradenoma during rounds at the hospital. She was super nervous but fascinated at the same time; she knew it wasn’t dangerous but wanted to learn more about its pathology. That moment reminded me how even small things in medicine can lead to significant learning experiences!
So yeah, while hidradenomas aren’t exactly on everyone’s radar, they matter in understanding skin pathology and improving patient care when it comes down to benign tumors. Plus, keeping an eye on these little bumps ensures we don’t miss anything more serious hiding underneath!
Comprehensive Pathology Outlines of Nodular Hidradenoma: Insights and Analysis in Dermatopathology
Nodular hidradenoma is a rare skin tumor that originates from the sweat glands, specifically the apocrine type. It’s one of those things you don’t hear about every day, but it totally deserves some attention! The tumor usually appears as a firm, painless lump under the skin. Commonly found on the scalp, face, and upper extremities, nodular hidradenomas can sometimes look like other types of skin growths, which makes diagnosis a little tricky.
The thing is, while they are mostly benign, understanding their pathology is crucial for proper treatment and management. You’ll often find these tumors in young adults or middle-aged individuals. They might not be life-threatening, but they can still cause concerns due to their appearance or discomfort.
- Histological Features: When you take a closer look at these tumors under a microscope, you’ll see they are composed of dermal nodules made up of epithelial cells that resemble sweat gland structures. There’s usually a mix of different types of cells here—some that look typical and some that might seem atypical.
- Clinical Presentation: Patients typically present with solitary nodules that may vary in size from small (like a pea) to several centimeters across. Sometimes they can be mistaken for sebaceous cysts or even lipomas!
- Differential Diagnosis: It’s super important to differentiate nodular hidradenoma from other conditions like adnexal carcinomas or even keloids based on its clinical and histological features because misdiagnosis can lead to improper treatments.
You know what’s interesting? Even though these tumors are benign, there have been very few cases noted where they turned malignant or recurred after surgical removal. So while most people go in for surgery and come out just fine, it’s always best to keep an eye on any changes post-op!
Treatment usually involves excision of the tumor. It’s important to ensure clear margins during surgery to minimize the risk of recurrence. And speaking of surgery—after dealing with my own pesky cyst back in college, I remember feeling nervous yet relieved when it was finally out! That sense of closure really does wonders for your peace of mind.
The clinical significance of understanding nodular hidradenoma can’t be overstated. For dermatopathologists and healthcare providers alike, having solid insights into this entity helps ensure accurate diagnoses and appropriate patient management strategies.
In short, while nodular hidradenoma might not sound like the most dramatic topic in dermatology; it’s definitely one worth knowing about! It brings together aspects of histology, diagnosis, and patient care—all vital pieces in the puzzle that is skin health.
Poroid Hidradenoma Pathology: Insights into Diagnosis, Histopathological Features, and Clinical Implications
Poroid hidradenoma is a rare type of skin tumor that arises from sweat glands, specifically the **apocrine glands**. It’s one of those things you might not hear about every day, but it’s essential to understand its pathology, diagnosis, and what it all means in clinical practice. Let’s break it down together.
First off, diagnosing poroid hidradenoma can be a bit tricky. These tumors often present as small, painless nodules on the skin—usually on the trunk or extremities. When you see one, it often looks like your standard benign growth. However, it helps to know that they can sometimes mimic other skin conditions. That’s why getting an accurate diagnosis is key. Dermatologists usually rely on a combination of physical examination and imaging techniques.
When you dig deeper into the histopathological features, you find that poroid hidradenomas have distinct characteristics under the microscope. These tumors are made up of two main cell types: **poroid cells** and **basaloid cells**. What’s intriguing is how these cells arrange themselves like lots of little clusters or nests. They can even form ducts resembling sweat gland structures!
Here’s a fun fact: during histopathological evaluation, these tumors may show some **cystic spaces**, which adds to their variety in appearance. Clinicians look for these features when examining tissue samples.
Now let’s get into clinical implications because this is where things get interesting. While poroid hidradenomas are mostly benign, there are some important points to consider:
- Potential for recurrence: Though they’re not cancerous, these tumors can come back after surgical removal.
- Differential diagnosis: They need to be distinguished from other similar lesions like basal cell carcinoma or melanomas for appropriate management.
- Surgical excision: This is usually the recommended treatment since most people want to get rid of them once they notice them.
You know what really drives home this point? A friend of mine had a poroid hidradenoma removed from her arm last year. The doctor explained everything thoroughly—about how rare they are and what to expect post-surgery—and honestly? It made her feel so much better knowing she was in good hands with someone who understood all those little details.
So yeah, while poroid hidradenoma isn’t something that most people think about daily, understanding its pathology gives us better insight into diagnosis and treatment options. It emphasizes the importance of vigilance—both by healthcare professionals and patients—when it comes to skin health!
Alright, so let’s chat about hidradenomas. It’s a bit of a mouthful, huh? But these little guys are actually pretty interesting when you dig into what they are and why they matter in the world of pathology.
So, basically, a hidradenoma is a type of tumor that forms in the sweat glands. They’re usually benign, meaning they don’t spread like cancer does. But just like that friend who shows up uninvited at your party, they can still be annoying. They often pop up on your skin, especially in areas like your armpits or groin. And if you’ve ever had one removed—ouch! Even though it’s not life-threatening, getting one taken out can feel quite invasive.
Now, I remember this one time my buddy had a bump on his back that he thought was just a harmless pimple. He kept picking at it until it started to hurt more than usual. Turns out it was a hidradenoma! I mean, who knew something that sounds so technical could lead to such drama over something seemingly small? It made me realize how important it is to pay attention to what’s going on with our bodies—sometimes those little nuisances are trying to tell us something more.
Clinically speaking, understanding hidradenomas is vital for doctors because even though they’re mostly harmless, differentiating them from other skin issues is key to proper treatment. You don’t want to confuse them with malignant tumors or other skin conditions—definitely not! This is where pathology comes into play; examining tissue samples helps doctors figure out what they’re dealing with and how best to handle it.
And you know what? The more we learn about these conditions—even the obscure ones—the better equipped we are as patients and healthcare providers. It gives us insight into the complexities of our own bodies and how they can sometimes surprise us in unexpected ways.
In the end, while hidradenomas might not be something you chat about over coffee (unless you’re really in the mood for dermatology gossip), their presence reminds us of the intricate dance within our skin and tissues—always doing their thing, even when we aren’t paying much attention.