You know how everyone used to freak out about germs? Like, all those hand sanitizers and antibacterial wipes? Well, they were kinda onto something. In the battle against stubborn little buggers like MRSA, those sanitizers aren’t always the superheroes we thought they’d be.
Seriously, MRSA—methicillin-resistant Staphylococcus aureus—sounds like something out of a sci-fi flick, right? But it’s real. It’s a type of bacteria that just doesn’t care about antibiotics. It’s got this wild talent for shrugging off meds that used to work like magic.
Imagine a tiny villain that keeps evolving, dodging every attack thrown at it. It’s not just annoying; it can be downright dangerous! So let’s chat about what MRSA does in our bodies and why it’s such a big deal in the world of antibiotic resistance. Buckle up; it’s gonna be an informative ride!
Understanding the Mechanisms of MRSA Resistance: Insights from Microbial Science
Well, let’s talk about **MRSA**, which stands for Methicillin-Resistant Staphylococcus Aureus. It’s a nasty little bug that’s quite the troublemaker in hospitals and communities. The thing is, it’s resistant to many antibiotics, which makes treating infections tricky. So, how does it do that? Let’s break this down.
First off, MRSA belongs to a family of bacteria called **Staphylococcus**, and it’s known for causing skin infections, pneumonia, and even more severe issues like bloodstream infections. Basically, MRSA has some clever tricks up its sleeve that help it survive where other bacteria would fall flat.
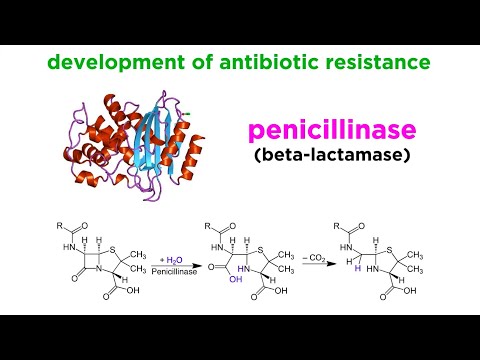
One major mechanism of resistance is the **production of beta-lactamase enzymes**. These little enzymes break down antibiotics like penicillin and methicillin. Imagine having a shield that deflects arrows—this is kind of what beta-lactamase does to certain meds.
Another sneaky tactic is related to its **cell wall structure**. MRSA alters its cell wall so antibiotics can’t latch on effectively. It’s like wearing spiked armor; the antibiotics just bounce right off! This process involves proteins known as **penicillin-binding proteins (PBPs)** that MRSA modifies so they don’t bind with the drugs anymore.
And here’s where things get even trickier: MRSA can also pick up genetic material from other bacteria! This means it can learn new resistance traits really fast—a bit like getting tips from your friends on how to win a video game level.
Now let’s touch on something called **biofilms**. These are protective layers that bacteria form when they stick to surfaces—like medical devices or even your skin when you have an open wound. Biofilms can shield them from both your immune system and the action of antibiotic treatments. It’s like throwing up walls around a fort; no one gets in, not even the good guys!
You might be wondering why all this matters. Well, if we don’t find ways to combat MRSA and similar resistant strains, we could find ourselves in a situation where common infections become lethal again—a real throwback to the pre-antibiotic era.
So how do researchers tackle this? They’re diving deep into microbial science! Some are searching for new antibiotics while others study how existing ones work against these resistant strains. There’s also a big push towards understanding our own immune responses better because sometimes it’s not just about the drugs; it’s about helping our body fight back too!
In summary:
- MRSA is resistant to many antibiotics.
- It produces beta-lactamase enzymes that degrade certain antibiotics.
- The bacterium alters its cell wall structure to evade drug action.
- It can accept genetic material from other bacteria for new resistance traits.
- Biofilms provide extra protection against treatments.
It’s pretty wild stuff when you think about it! Understanding these mechanisms is crucial for overcoming antibiotic resistance and keeping those pesky germs at bay. So yeah, there’s still lots of work ahead, but researchers are on it!
Understanding MRSA Antibiotic Resistance: Implications for Modern Medicine and Scientific Research
So, let’s talk about MRSA, which stands for Methicillin-Resistant Staphylococcus aureus. It’s a type of bacteria that’s become a big deal in the world of medicine, mainly because it doesn’t respond to many common antibiotics. Imagine you’ve got a persistent little brat that refuses to listen, no matter how many times you tell it what to do—that’s MRSA for you.
This bacteria isn’t just hanging out in random places; it thrives in hospitals and communities and can cause a bunch of infections. Sometimes it shows up as a skin infection, like those nasty boils or abscesses you might have seen. But here’s where it gets serious: MRSA can also dive deeper and lead to pneumonia or bloodstream infections. Seriously, these things are no joke!
Now, let’s get into how MRSA has become so stubborn against our trusty antibiotics. Basically, this resistance happens when bacteria change or mutate in ways that allow them to survive even when antibiotics are around. In the case of MRSA, it’s got this gene called mecA that helps it make a new protein which avoids being attacked by methicillin. It’s like wearing an invisible cloak!
But why does this matter? Well, antibiotic resistance is super concerning for modern medicine because it makes treating infections harder and takes longer. Here are some key implications:
- Longer hospital stays: When MRSA shows up in hospitals, patients might need more time to heal.
- More complicated treatments: Doctors may have to resort to using stronger—or less preferred—antibiotics.
- Increased costs: Treatments get pricier, not just because of medication but from prolonged care too.
- Higher risk of complications: Infections can spread or worsen if not treated quickly and effectively.
Okay, so what about the science behind all this? At the root of MRSA’s resistance are factors like natural selection. You know how not every plant survives when things get rough? Same goes for bacteria! Those little guys evolve over time and develop defenses against whatever tries to take them out.
Plus, there’s also antibiotic misuse happening everywhere! Over-prescribing antibiotics when they’re not needed creates an environment where resistant bacteria can thrive. Imagine planting seeds in your garden but only watering the weeds—you’ll end up with more weeds than flowers!
Remember that time you had an infection and got prescribed antibiotics? If they were given unnecessarily or if you didn’t finish your entire course (we’ve all been there), some bacteria might still be lurking around ready to adapt and multiply.
And here’s where research comes into play! Scientists are constantly looking for new ways to combat these resilient bugs through better treatments or understanding their biology more deeply. Vaccine development is one area getting attention—if we can prevent infections from happening in the first place, that would help reduce reliance on antibiotics.
So yeah, MRSA is like that sneaky foe we didn’t see coming—a reminder that our fight against bacterial infections is ongoing and requires teamwork between doctors, researchers, and patients alike! Understanding how these bugs function helps us pave the way forward for better medical care while keeping those pesky germs at bay.
Comprehensive MRSA Treatment Guidelines: Evidence-Based Approaches for Effective Management
MRSA, which stands for Methicillin-Resistant Staphylococcus Aureus, is like that annoyingly persistent friend who just won’t leave your party. It’s a type of bacteria that has become resistant to many antibiotics, making it a real headache when you try to treat infections. The pathophysiology of MRSA involves some complex stuff, but let’s break it down.
Basically, MRSA is a strain of Staphylococcus aureus, a common bacterium found on our skin and in our noses. Most people carry it around without any issues. But when it breaks through our defenses—like cuts or abrasions—it can cause serious infections. What makes MRSA particularly troublesome is its ability to resist methicillin and other similar antibiotics. That happens because of changes in its genetic material!
Now, you might be wondering why this matters so much. Well, as more bugs learn to dodge the drugs we throw at them, it becomes tougher for doctors to fix something as simple as an infection. Standard treatments may not work anymore, making what should be a straightforward recovery process way more complicated.
When we talk about treatment guidelines, we’re looking at strategies based on solid research and real-world results. There are some key elements that come into play:
- Diagnosis: You need a proper assessment first—knowing whether it’s MRSA or something else changes the game.
- Antibiotic Therapy: Options include medications like vancomycin or linezolid that are specifically effective against MRSA.
- Infection Control: This means keeping the infection from spreading by using good hygiene practices both at home and in healthcare settings.
- Surgical Intervention: Sometimes infections require draining abscesses on top of taking antibiotics; you can’t just rely on meds alone!
Speaking of antibiotic therapy, the choice can depend on how severe the infection is as well as where it’s located in the body. For example, skin infections might get treated differently from pneumonia caused by MRSA.
But here’s where things can get dicey—sometimes patients don’t respond to initial treatments because resistance patterns change! That’s why ongoing monitoring is super important.
It’s kind of scary when you think about how quickly bacteria adapt. Like they’re always one step ahead! So health professionals often lean on evidence-based approaches that are constantly updated with new research findings.
And if you’re ever in doubt about your own health or what you can do about preventing an infection? Seriously just consult a healthcare professional! They have tons of resources and knowledge at their disposal.
So there you have it—just like any good story worth telling, dealing with MRSA takes careful planning and smart decisions based on solid science!
Okay, so let’s chat about MRSA, which stands for Methicillin-resistant Staphylococcus aureus. Sounds like a mouthful, right? Well, it’s actually pretty interesting once you dig into it.
MRSA is a strain of a common bacteria, Staphylococcus aureus—basically a little guy that hangs out on our skin and in our noses without causing much trouble. But when it decides to turn rogue and sets off an infection? That’s where the drama begins. It’s not just any infection; this little troublemaker is super tough because it doesn’t give in to common antibiotics like methicillin.
So here’s where the story gets intense: this antibiotic resistance is like watching a superhero evolve into an even stronger villain. You see, MRSA developed its resistance over time, mostly because of how we use antibiotics in medicine and sometimes even in livestock farming. When antibiotics are used too much or not taken properly, bacteria can figure out ways to survive them. It’s like they’re taking notes on how to become invincible!
I once heard about someone getting a pretty nasty MRSA infection after surgery—totally unexpected! They were recovering from what seemed like a routine procedure but ended up with this resilient bacteria wreaking havoc. It just goes to show how sneaky MRSA can be.
The pathophysiology behind MRSA is all about its ability to evade the immune system and resist treatment. This bacterium produces certain proteins that help it hide from our body’s natural defenses while also blocking the action of antibiotics aimed at killing it off. It’s clever, right? Most infections cause inflammation and pain as your body fights back, but with MRSA, it can go undetected or just spiral out of control really fast.
And here’s another twist: as MRSA spreads through hospitals or community settings (you know when someone shares their germs way too freely?), it creates a real headache for healthcare providers trying to manage infections that don’t respond to standard treatments.
So what can we do about all this? Well, while researchers are working hard on new antibiotics and treatments, there’s also a big push on proper hygiene practices—like washing your hands regularly and being mindful with antibiotic prescriptions so we don’t give these bacteria more chances to become resistant.
In short, MRSA is one of those reminders that while science has done amazing things in medicine, nature has its own set of tricks up its sleeve! We need to stay vigilant about how we treat infections because who knows what else might be lurking around the corner with these evolving pathogens?