You know when you hear someone wheeze and it sounds like a miniature harmonica in trouble? It’s kinda funny, but not really! Wheezing is more than just a quirky sound; it’s a serious signal from our lungs.
Imagine this: you’re running late for work, and all of a sudden, your chest feels tight. You try to catch your breath, but that little wheeze comes creeping in. It’s annoying, right? But there’s a whole story behind that sound.
So, what’s actually going on inside when you wheeze? Like, why does it happen? It turns out there are some pretty interesting mechanisms at play. And understanding them can really change how we think about our health.
Buckle up as we unravel the mystery behind wheezing! You might find it more fascinating than you thought!
Comprehensive Guide to the Pathophysiology of Asthma: Downloadable PDF Resource for Scientific Study
Asthma, oh boy, it’s a tricky condition, isn’t it? It really messes with your breathing. Basically, the pathophysiology of asthma involves a lot of different factors that come together to make your airways super sensitive. Here’s the lowdown.
When you think about asthma, picture your airways like a garden hose. In a healthy state, water flows easily through that hose. But if there’s something blocking it or if the hose itself starts to swell up, you’ve got problems! That’s kind of what happens with asthma.
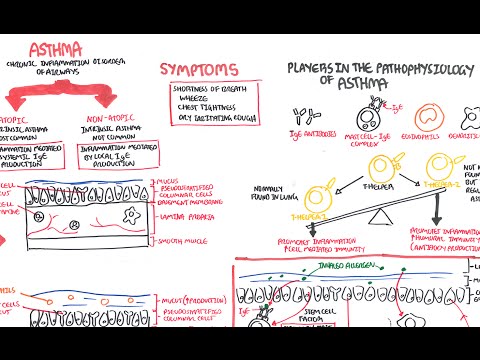
So, what really goes down in the airways? First off, there are these cells called *mast cells*, which are like the alarm system for your body. When they sense an allergen—like dust mites or pollen—they go haywire and release all sorts of chemicals (histamines, for instance). This leads to inflammation and narrowing of those air passages.
Here’s where it gets interesting: you also have smooth muscle around those airways. In asthma patients, those muscles tend to squeeze more than usual when triggered by certain stimuli. So now you’ve got swollen tissues and tight muscles making it even harder to breathe!
And then there’s mucus production—oh boy! A normal response can turn excessive in asthmatics. Your body tries to protect itself by creating more mucus when there’s an irritant around but sometimes it gets carried away. Imagine trying to breathe through a straw that keeps getting clogged; not fun at all!
It doesn’t end there; there’s also airway remodeling. Over time, repeated inflammation can change the structure of those airways forever—like turning that flexible garden hose into something stiff and unyielding. Scary stuff!
But let’s talk about symptoms: wheezing is one of them! It sounds like that high-pitched whistle when someone breathes out forcefully while their airway is narrow. So when you hear someone wheeze? That’s actually an indicator that their lungs are struggling.
Now if we shift gears a bit and look at management: things like inhalers are key players here. They help open up those tight muscles and reduce inflammation—a bit like giving that garden hose some much-needed oil!
And although we’re dealing with something serious here, it’s vital to remember individual experiences vary widely among people with asthma. Some might have mild symptoms occasionally while others could find themselves struggling daily.
In sum:
- Mast cells trigger inflammation upon exposure to allergens.
- Smooth muscle contraction narrows the airways further.
- Mucus overproduction clogs up everything.
- Airway remodeling changes lung structure permanently over time.
- Wheezing indicates troubled breathing during episodes.
Sometimes I think back on my young neighbor who used to struggle with his inhaler before soccer practice—it was just heartbreaking watching him miss out on games because he couldn’t catch his breath amid all the excitement.
In short, understanding this pathophysiology helps not only in treating asthma but also in finding ways for patients to thrive despite it! Whether it’s learning about new treatments or simply recognizing triggers—it’s all about making life easier for those who live with this condition every day.
Comprehensive Flowchart on the Pathophysiology of Asthma: Key Mechanisms and Processes in Respiratory Science
So, let’s get into the nitty-gritty of asthma and why it causes that wheezing sound we all may have heard. You know, that tightness in the chest… it’s not just annoying; it’s a real thing happening in your lungs. The pathophysiology of asthma involves a bunch of players: inflammation, bronchoconstriction, and even some structural changes in your airways. So here’s a breakdown without getting too technical.
Airway Inflammation
Asthma usually starts with inflammation of the airways. That means your body is reacting to something like allergens or irritants (like smoke). When this happens, immune cells jump into action. They release substances that can make the airways swell up and get super sensitive. Think of it as your body being overprotective.
- Mast Cells: These are like the soldiers of inflammation. They release histamine and other chemicals that cause itching and swelling.
- Eosinophils: Another group of immune cells that contribute to inflammation, particularly in those who have allergic asthma.
Bronchoconstriction
Okay, so once inflammation kicks in, the muscles around your airways can tighten up. This is what we call bronchoconstriction. It literally narrows down those passages you use to breathe—making it harder for air to flow. You might feel tightness if you’re asthmatic because of this.
- Triggering Factors: Exercise or cold air can induce this tightening response!
- Nerves: The nervous system also plays a role here; certain signals can make those muscles squeeze even more.
Mucus Production
As if things weren’t complicated enough! Asthma often comes with an increase in mucus production, which can further clog up those narrowed airways. Imagine trying to breathe through a straw that’s been dipped in slime—gross but pretty accurate!
- Mucous Glands: These glands go into overdrive when there’s inflammation.
- Mucus quality: Sometimes it’s thick and sticky, making it even harder to clear from your lungs!
Airway Remodeling
This part usually takes more time but can significantly impact long-term health. If asthma isn’t managed well over time, repeated cycles of inflammation can lead to structural changes in the airway walls. Basically, they thicken and may lose some elasticity.
- Smooth Muscle Hypertrophy: The muscle lining gets bigger as a response to constant tightness.
- Epithelial Changes: The surface layer may become more fragile or change its characteristics altogether.
The Wheezing Sound
Now here’s where things come full circle! The wheezing you hear during an asthma attack is basically caused by airflow being obstructed as you try to breathe through those narrow airways filled with mucus while they’re inflamed… it’s like trying to sip soda with a boba straw!
You see? Asthma isn’t just one thing but rather a mix of different processes coming together—each contributing to how you feel when you’re having an attack. Managing these elements means thinking about the triggers, using medication correctly (like inhalers), and keeping everything under control.
So yeah, understanding asthma’s pathophysiology helps us appreciate why it’s essential to pay attention if you or someone close has it! It’s not just about wheezing; there’s a whole lot going on inside those lungs!
Understanding the Pathophysiology of Wheezing in Asthma: Insights for Scientific Research
Wheezing is that whistling sound we hear when someone breathes, especially during an asthma attack. It’s more than just a noise, though; it tells us something important about what’s happening in the lungs. When you think of asthma, imagine your airways are like garden hoses. Sometimes they get squeezed and blocked. That’s basically what wheezing is: air struggling to get through narrowed pathways.
Asthma can be triggered by a bunch of different things—maybe pollen in the air, pet dander, or even a strong smell from cleaning products. These irritants cause inflammation in the airways. Your body gets all defensive and sends out immune cells to fight off these invaders. This is where things start to go a bit haywire.
So, when your airways become inflamed, they get swollen and filled with mucus. It’s like trying to push toothpaste through a blocked tube! The muscles around the airway walls also tighten up—a response that can feel pretty scary when you’re gasping for breath.
The pathophysiology of wheezing involves a few key mechanisms:
- Inflammation: This is the main player! When something irritates your airways, inflammation kicks in.
- Mucus Production: Your body goes into overdrive producing mucus, which further blocks airflow.
- Bronchoconstriction: The muscles around your airways contract too much. It makes those tubes extra tight.
Imagine being at a concert and someone keeps pushing against you from behind—that’s how it feels when your airway tightens up!
Research into this wheezing phenomenon is super important because understanding these mechanisms helps scientists develop better treatments. For instance, some medications target that inflammation directly, while others help relax those tight muscles around the bronchial tubes.
You know how people often talk about allergies? Well, there’s research showing that allergic reactions can worsen asthma symptoms too—like adding fuel to a fire! The presence of allergens can amplify that inflammatory response even more.
But it’s not just about allergens; other factors come into play as well:
- Exercise: Some folks experience exercise-induced asthma where physical activity triggers wheezing.
- Coughing: A persistent cough often accompanies wheezing; it tries to clear those blocked passages out.
When you hear someone wheeze or cough like this, it’s often because their body is really struggling to breathe properly. It’s crucial for researchers and healthcare providers to keep digging deeper into these mechanisms so we can find new ways to help people manage their asthma effectively.
So next time you hear someone wheeze or feel out of breath yourself, remember there’s a whole lot happening behind the scenes in your lungs—something not many think about until they’re gasping for air! By learning more about how all this works, we get closer to making life easier for anyone dealing with asthma and wheezing challenges daily.
Wheezing, huh? It’s one of those things that many people might have experienced at some point. I mean, you know that wheezy sound when someone is having a hard time breathing? It’s more than just a noise; it tells us a whole story about what’s going on inside the lungs.
So, here’s the deal: when we breathe, air travels through our airways – those tubes in your lungs. But sometimes, these airways get all cranky and start narrowing due to inflammation or other funky stuff. This could be triggered by allergies, infections, or even asthma. Then, when air tries to push through those tight spaces, you get that unmistakable wheeze. It’s like trying to squeeze toothpaste out of a tube that’s too small. Frustrating, right?
I remember this one time at a family gathering—my little cousin was running around all energetic when suddenly she stopped and started wheezing. Everyone kinda froze for a moment; it was scary! Turns out she had an allergy flare-up. And while we were worried about her, it just highlighted how important breathing is and how something so simple can go haywire so quickly.
What’s super interesting is the underlying mechanisms that cause wheezing are actually pretty complex. When you have inflammation in your airways—like what happens with asthma—the smooth muscles around them tighten up (think of them as tiny bouncers at a club). These bouncers are generally chill but can go into overdrive because of various triggers like smoke or cold air. The result? Less space for air to flow!
And let me tell you—it doesn’t just stop at the wheeze itself. Over time, constant wheezing can lead to other problems like reduced lung function or even chronic conditions if it’s not managed well. That’s why understanding what’s happening in our bodies during these episodes matters so much.
Honestly, it amazes me how our bodies communicate with us through these sounds and sensations. A little wheeze might seem trivial in isolation but can hint at bigger health issues lurking beneath the surface. Life has this funny way of reminding us about what we often take for granted—like simply being able to breathe freely without any weird noises coming from our chests.
Just goes to show how crucial it is to listen and respond when our bodies speak up—whether through wheezing or any other sign they give us!