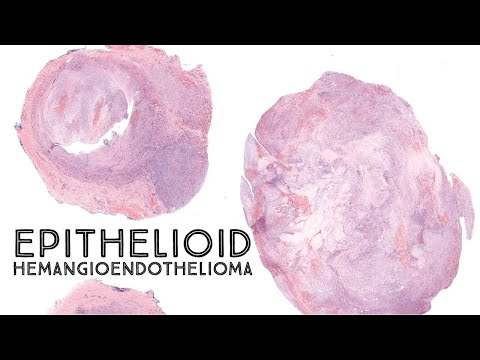
So, picture this: you’re chilling at a party, and someone brings up the name “Epithelioid Hemangioendothelioma.” You glance around to see if everyone else is as confused as you are.
Well, trust me, you’re not alone. That name sounds like something out of a sci-fi movie, right? But behind that hefty title lies something pretty interesting—medically speaking, of course.
Imagine you’re sitting in your doctor’s office, and they mention this rare tumor. It’s not exactly the kind of small talk people make at brunch! But here’s the deal: understanding these kinds of conditions can actually help demystify a lot about cancer and how our bodies work.
I mean, who doesn’t want to know more about what makes us tick? Epithelioid Hemangioendothelioma might sound daunting at first, but unraveling its insights can lead to some fascinating discoveries about our health and pathology. So let’s dig into it!
Exploring the Impact of EHE: Organs Typically Affected by Epithelioid Hemangioendothelioma
Epithelioid hemangioendothelioma (EHE) is a rare vascular tumor. It’s all about those cells that line the blood vessels. When things go wrong, they turn into these tumors, which can pop up in various organs. Now, let’s break down the organs that are often affected by EHE.
Liver: The liver is one of the most commonly impacted organs. Around 30-40% of EHE cases show up here. Patients might not experience symptoms until the tumor has grown quite a bit. And that’s really concerning because it can lead to serious complications if not caught early.
Lungs: Next on the list is the lungs, where about 20-30% of cases are found. This can cause all sorts of breathing issues and might be mistaken for other lung diseases. It’s like playing a game of hide and seek with your health!
Soft tissues: EHE can also pop up in soft tissues around the body, such as in the extremities or trunk. This can lead to painful swellings or masses you’re just not sure what to make of, especially if they suddenly increase in size.
Bone: Bone involvement is less common but it does happen. When EHE makes its way into bones, it can lead to bone pain or fractures without any clear reason—super frustrating!
Bulging into your everyday life like this makes EHE tricky to deal with because symptoms vary so much between individuals. Many people just chalk up their symptoms to normal aches and pains instead of seeking help right away.
So why does this matter? Well, knowing which organs are typically affected helps doctors make better decisions when you present symptoms that don’t seem right. Early detection is key! The earlier EHE is discovered, the better chances there are for effective treatment.
In short:
- Liver: Most common site; often asymptomatic until later stages.
- Lungs: Causes breathing issues; can get confused with other lung diseases.
- Soft tissues: Can appear as painful masses; size may increase unexpectedly.
- Bone: Rarely involved but can cause unexplained pain or fractures.
Understanding these impacts really sets the groundwork for effective care and management strategies moving forward! So keep an eye on those symptoms—it could make a world of difference down the line!
Understanding the Growth Rate of Epithelioid Hemangioendothelioma: Insights from Oncology Research
Epithelioid hemangioendothelioma (EHE) is quite a mouthful, huh? It’s a rare and tricky tumor that arises from endothelial cells, which line blood vessels. You might be wondering, “What does that even mean?” Let’s break it down together.
First off, the growth rate of these tumors can vary quite a bit. Some people might have slow-growing tumors that just kind of hang out for years without causing much fuss. Others, though, can experience more aggressive forms that pop up and spread faster. It’s like waiting for a pot to boil—some days it feels like forever, and others you turn around and BAM! It’s boiling over.
According to research from oncology studies, there are several factors influencing the growth rate of EHE:
- Location of the tumor: Where the tumor develops can really change things. If it’s in an area with lots of blood supply, like the liver or lungs, it might grow faster.
- Patient age: Younger patients often have different growth patterns compared to older adults. Kids’ bodies sometimes react differently, leading to varied rates of tumor development.
- Genetic factors: There are some gene alterations linked with EHE that can impact how quickly these tumors grow. Understanding your DNA isn’t just about learning who your great-great-grandparents were!
- The immune response: Our bodies’ defenses play a crucial role too! A stronger immune response might help keep things in check while a weaker one could let these tumors run wild.
It’s pretty fascinating how all these different components play together. Just imagine a dance party where some folks are dancing slowly and others are breaking out their best moves—it creates quite the scene!
Now let’s talk about those pathology insights. Doctors use various methods to study EHE under the microscope which helps them understand its growth better. They look for specific characteristics like cell shapes and structural patterns that can give clues on aggressiveness.
One interesting thing researchers have noted is how EHE can sometimes mimic other diseases. So if you were at a party and saw someone who looked exactly like your buddy but was acting all weird—you’d start to wonder if something else was going on too! That confusion can delay diagnosis or lead to misinterpretation.
Another point worth mentioning is treatment options available for EHE patients. While surgery is often the go-to solution if it’s localized and hasn’t spread too much—a lot depends on how fast it grows and where exactly it’s hanging out in your body.
In terms of survival rates? Well, statistics do indicate that those with low-grade EHE generally fare better than those with more aggressive versions. It’s kind of like playing poker: if you’ve got good cards (or in this case, good health signs!), you’re usually in for a better outcome!
So there you have it! Understanding epithelioid hemangioendothelioma’s growth rate isn’t just about numbers; it’s about recognizing the unique story each patient tells through their pathology and personal journey through treatment. Keep asking questions; that’s how we learn more every day!
Understanding the Distinctions Between EHE and Hemangioma: A Scientific Overview
Sure thing! Let’s break down the differences between Epithelioid Hemangioendothelioma (EHE) and hemangiomas in a way that’s, you know, easy to digest.
EHE and hemangiomas might sound similar because they both involve blood vessels and can appear as tumors, but they have some real distinctions that are important to understand.
Firstly, EHE is a rare tumor that comes from endothelial cells. These cells line the blood vessels. It’s not just a lump; it can behave more aggressively than your average tumor. EHE can occur in various organs like the liver, lungs, or soft tissues. While it can be benign in some cases, it has the potential to spread or metastasize.
On the other hand, hemangiomas are usually benign tumors made up of a tangle of blood vessels. You often see these on the skin or in superficial tissues. They’re super common in babies and often go away on their own over time—like, poof! They just fade.
Now let’s get into some specifics:
Another key point is treatment strategies—EHE may require surgical removal along with possible additional therapies if it’s aggressive or metastatic. With hemangiomas? Most doctors recommend just watching and waiting since they often resolve without any intervention.
So you see? While both involve blood vessels and might look similar at first glance, they really do belong to different worlds when it comes down to their behavior and treatment.
Honestly speaking, understanding these differences can feel daunting at times—especially if someone close to you is diagnosed with either condition. Just remember: having clear information really helps make sense of what’s going on!
So, let’s talk about something that might sound super complex but is actually pretty fascinating. Epithelioid hemangioendothelioma, wow, what a mouthful, huh? It’s one of those rare tumors that pops up in blood vessels. You know, it’s like when you’re wandering around a cool old town and you find something super interesting but kinda rare—like a hidden gem among the usual tourist traps.
I remember hearing about it during a medical seminar I went to once. There was this passionate speaker who shared stories of patients dealing with this condition. He spoke with such heartfelt emotion that you could practically feel the weight of their struggles in the room. It really struck me; these are real people affected by this rare disease.
Now, epithelioid hemangioendothelioma (let’s just call it EH for short) is quite the tricky character. It’s not benign—you definitely don’t want to underestimate it. But at the same time, it’s not your classic aggressive cancer either. It has this weird way of letting people hang on for a while before making its impact felt.
When we look at pathology insights into EH, there are some key features that stand out. For instance, pathologists often spot these distinct epithelioid cells under a microscope. They can be arranged in clusters or nests—almost like little communities trying to thrive inside your body! And then there’s this thing called vascular invasion where these cells kind of sneak into blood vessels. It’s like they’re trying to hitchhike around your system.
One striking finding is how varied the behavior of this tumor can be after it’s diagnosed. Some folks may live years without significant issues, while others might face more challenging paths—all depending on how aggressive the tumor is and where it decides to take root in the body.
Research continues to unravel its mysteries and there’s still so much we don’t know yet! But that’s what makes science exciting—you never quite know what you’ll uncover next! Just thinking about it all makes me feel both hopeful and curious about how our understanding evolves over time.
So yeah, while terms like epithelioid hemangioendothelioma might sound intimidating at first glance, digging deeper reveals stories of resilience and discovery within healthcare that resonate with so many people out there facing tough battles every day.