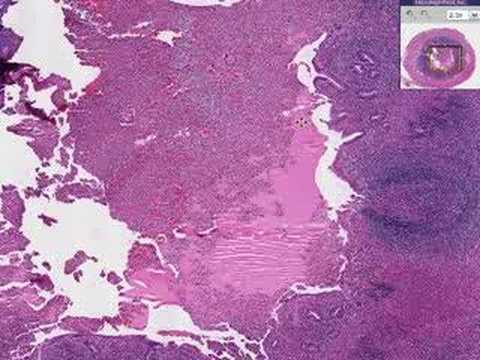
So, you know when someone mentions appendicitis, and you can’t help but cringe just a little? I mean, who wants to think about their insides going haywire, right? But here’s a wild thought: have you ever considered that the appendicitis saga is like a secret drama unfolding in our bodies? Yeah, seriously!
Picture this: your appendix is like that quiet kid in the back of the classroom. Everyone forgets about it until it suddenly decides to throw a fit. That’s when things get messy, and boom—it’s showtime!
In this chat, we’re going to peek behind the curtains of this unexpected performance. We’ll dive into the histological details—fancy talk for how tissues look under a microscope—and see what really goes down during an appendicitis attack. It’s like getting VIP access to a medical mystery you never knew existed! So grab your snacks (not too heavy though!), and let’s unravel the story together.
Essential Histologic Findings for Accurate Diagnosis of Acute Appendicitis in Surgical Pathology
Let’s talk about acute appendicitis and what pathologists look for under the microscope to figure out if that’s what’s going on. You might not think of histology every day, but it plays a huge role in diagnosing conditions like appendicitis. I’ll break down some essential findings you’d find in the tissue samples.
Firstly, when the tissue gets sliced up for examination, the most significant sign of acute appendicitis is neutrophilic infiltration. Neutrophils are a type of white blood cell that’s basically like your body’s first responder against infection. If you see a bunch of these cells invading the appendiceal wall, it’s a strong indicator that something’s wrong.
Then there’s mucinous degeneration. This is when mucous-producing cells swell up and become dysfunctional. When pathologists spot this in an appendix sample, they take note. Mucin can block ducts and contribute to inflammation.
Another thing that pops up is necrosis. Basically, this means some of the cells are dying off because they’re not getting enough blood flow. In cases where necrosis is apparent, it tells us that this isn’t just minor inflammation; it’s serious and could lead to complications.
- Subserosal edema: You might find swelling below the surface area of the tissue. This can indicate an ongoing inflammatory process.
- Lymphoid hyperplasia: Sometimes before things get really bad, you might see an increase in lymphoid follicles within the mucosa. It can be like a warning sign that trouble is coming.
- If abscesses form: That brings a whole new level of complication! They can show localized collections of pus that will need urgent attention.
Now let me tell you a quick story here—it was actually my buddy’s grandfather who had his appendix burst because he brushed off his stomach pain for too long. The doctors said if only he had sought help sooner! That kind of advanced inflammation often leads to more severe symptoms like fever or nausea but catching it early with histological insights could really make a difference.
But here’s where things get tricky—there are other conditions that can mimic appendicitis on histology, such as colitis or even tumors! So pathologists need to put on their detective hats and analyze all aspects carefully: location of neutrophils, patterns in cell arrangement, and so forth.
The key takeaway here? Acute appendicitis is all about those specific histologic features we’ve talked about—each one offering clues about what’s happening at a cellular level. So next time you hear someone mention appendicitis or see “histopathology” on a report, you’ll know just how crucial those little details can be!
Microscopic Features of Acute Appendicitis: A Comprehensive Analysis in Pathology
Sure! Let’s chat about the microscopic features of acute appendicitis. It’s a pretty fascinating topic when you dig into the details. You know, when someone has appendicitis, what’s happening on a cellular level is crucial for understanding how this condition develops.
Acute appendicitis is an inflammation of the appendix, and it’s often caused by a blockage in its lumen. This blockage can lead to all sorts of histological changes in the tissue. So, here goes:
Inflammatory Response
When the appendix becomes blocked, immune cells start to show up in large numbers. Basically, these cells are your body’s way of fighting infection and inflammation. You’ve got neutrophils – which are like tiny soldiers – rushing to the site first.
- Neutrophils: These are usually abundant in early appendicitis and can be found invading the epithelial layer of the appendix. Their presence indicates an acute inflammatory response.
- Lymphocytes: As you dig deeper into the infection, you might see more lymphocytes coming into play later on.
Tissue Changes
Now here’s where it gets interesting: with all that inflammation going on, there are noticeable changes in the tissue structure itself.
- Mucosal Edema: The lining inside the appendix gets swollen due to fluid accumulation. It’s kind of like when your ankle swells up after a sprain!
- Epithelial Loss: The epithelial cells may start to die off or become damaged due to inflammation—like they don’t stand a chance against those immune soldiers.
Pus Formation
One hallmark feature of acute appendicitis is pus formation, which you probably guessed! This is basically a mix of dead cells, bacteria, and debris.
- Pus: You often find it within the lumen of the appendix. It’s like a big sign that there’s an intense battle happening inside.
- Necrosis: In severe cases, part of the appendix wall might start breaking down due to ongoing damage.
Bacterial Involvement
You can’t really talk about acute appendicitis without mentioning bacteria! They really stir up trouble here.
- Bacteria Types: Common culprits include E.coli and other mixed flora that normally live in your gut but can cause chaos when they invade damaged tissues.
- Culture Results: Sometimes doctors will culture these bacteria during surgery or after removal to figure out what’s going on inside your body.
So basically, each microscopic feature tells its own part of this dramatic story—it’s like reading a really intense novel packed with twists and turns! Seeing how everything fits together gives us valuable insights into not just how appendicitis happens but also how our bodies respond at such tiny levels.
It’s wild thinking about all this stuff happening beneath our skin while we go about our day-to-day lives! And honestly, understanding these details helps doctors treat patients more effectively by recognizing early signs and tailoring treatments accordingly.
Understanding Appendix Pathology: Insights into Diagnosis and Treatment in Medical Science
Sure! Here’s a straightforward explanation of appendix pathology, focusing on things like appendicitis and how it’s diagnosed and treated.
The Appendix’s Role
Okay, so let’s start with what the appendix actually is. The appendix is this small pouch hanging off your large intestine. You might not think it has much importance, but some research suggests it plays a part in gut health. Still, it can also get into trouble—like when you develop appendicitis.
What’s Appendicitis?
Appendicitis happens when the appendix becomes inflamed. This inflammation can be due to various reasons, like blockages from stool or infections. Sometimes, it feels like someone kicked you in the stomach; other times it’s just a dull ache that intensifies over time.
Imagine you’re having a laid-back day and suddenly you feel this sharp pain in your lower right abdomen. It’s annoying and unsettling! This area is known as McBurney’s point—the spot where appendicitis pain usually centers.
Symptoms to Look For
Recognizing the symptoms is crucial because if left untreated, appendicitis can lead to serious complications. Typical signs include:
- Aching around your belly button that moves to the lower right side
- Nausea or vomiting
- Lack of appetite
- Fever
- A bloated belly
If you notice these symptoms, it’s best to see a doctor pronto!
Diagnosis: How Do They Figure It Out?
Doctors use a mix of physical exams and tests to confirm appendicitis. They’ll likely press on your stomach to check for tenderness. An ultrasound or CT scan might follow to visualize the appendix better.
But here’s where things get interesting: they can also look at the histology—the microscopic structure—of tissue samples. If they see signs of inflammation or infection under a microscope, it solidifies the diagnosis. This means they take a small piece of tissue from around your appendix during surgery for closer inspection.
Treatment Options
So if you have appendicitis, treatment usually involves surgery—specifically an appendectomy, which is just fancy talk for removing the appendix. Depending on how severe things are, doctors might even go for minimally invasive techniques using small cameras and instruments.
In some cases where inflammation isn’t extreme (or if they’re trying something non-invasive), antibiotics alone may suffice for treatment initially. But keep in mind; **surgery remains the most effective way** to prevent future complications.
Post-Surgery Considerations
After surgery, recovery generally goes smoothly for most people—but take it easy! Eating lighter foods can help ease you back into your routine without tension on your stomach area.
While complications are rare nowadays thanks to modern medicine and surgical techniques, some folks could still end up with infections or abscesses post-op. Just remember: staying alert and seeking prompt care if something feels off makes all the difference!
Wrapping It Up
In short, understanding appendix pathology could save you from unnecessary pain down the line! With clear symptoms and modern diagnostic tools at our disposal today (seriously amazing!), doctors have ways to tackle conditions like appendicitis effectively. So if you’re feeling that unmistakable ache in your abdomen? Don’t brush it off—get checked out!
So, appendicitis, right? It’s one of those things where you hear about someone getting their appendix out and you think, “Oh man, that sounds rough.” But have you ever thought about what’s actually happening inside your body when that goes down? A peek into the histological world can be pretty eye-opening!
Now, histology is just a fancy term for studying tissues. Imagine getting a close-up look at the tiny structures that make up your organs. When it comes to appendicitis, there’s this whole dramatic show happening at the microscopic level. The thing is, the appendix is like this little tube connected to your large intestine. Sometimes it gets blocked—maybe something as harmless as poop or even a foreign object. Once it gets blocked, bacteria jump in and start throwing a wild party.
It’s wild how quickly things can escalate! You might think it’s just an annoyance, but soon enough that blockage leads to inflammation—like an angry red firework show—but inside your body! Under the microscope, what you’d see are tons of immune cells piling up. These little soldiers are trying to fight off the infection. But here’s where it gets interesting: if they go overboard, they can cause tissue damage. That can make things worse before they get better.
You know what hit me while I was reading up on this? It reminded me of when I had my first bout of food poisoning. Just imagine your insides going from chill mode to full-on chaos: cramps, nausea—you name it. That feeling of being out of control totally resonates with what happens during appendicitis.
And here’s another thing—if treatment doesn’t happen quickly enough and that inflammation turns into an abscess or worse—perforation—then you’re looking at some serious complications. It really puts into perspective how important it is for us to listen to our bodies when they send us those “hey something’s not right” signals.
So yeah, histologically speaking, appendicitis reveals a lot about our body’s response mechanisms and reminds us how interconnected everything really is inside us. It’s kind of crazy how such a small organ can cause so much trouble! Next time you hear about someone having their appendix out or experiencing those sharp abdominal pains, maybe you’ll think twice about all those tiny cells doing their thing in a battle nobody else can see!