You know what’s weird? Your body has this tiny gland called the parathyroid, and it’s like the unsung hero of your health. But when it goes rogue, things can get pretty messy. Seriously.
Imagine having too much calcium in your blood—it sounds kinda cool, right? Like, “Look at me, I’m practically a walking milkshake!” But trust me, living like that isn’t as fun as it sounds. Hyperparathyroidism is like that unexpected guest who overstays their welcome at a party.
This condition messes with your bones, mood, and even how your kidneys function. It might sound complex, but let’s break it down together. We’ll chat about what’s going on inside your body and why you should care about this little hormone factory. So, hang tight!
Understanding Secondary Hyperparathyroidism: Pathophysiology, Diagnosis, and Treatment Options in Endocrine Science
So, let’s talk about this thing called **secondary hyperparathyroidism**. It sounds like a mouthful, right? But really, it’s about what happens when your body’s parathyroid glands go into overdrive because of low calcium levels. I mean, picture this: you’re going about your day when suddenly your body says, “Whoa! We need more calcium!” And then the parathyroids start pumping out parathyroid hormone (PTH) like there’s no tomorrow.
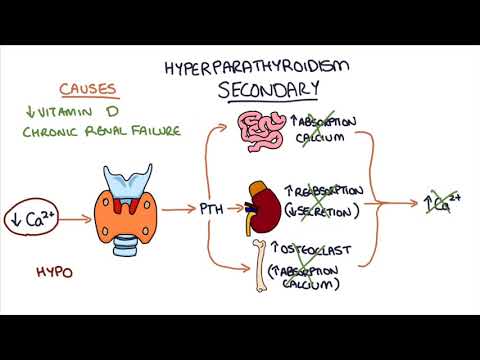
Pathophysiology is just a fancy way of saying how something works in the body when it goes wrong. In secondary hyperparathyroidism, usually it’s not the glands themselves that are the problem—they’re responding to some low calcium situation or maybe even high phosphate levels. This can happen with conditions like chronic kidney disease where your kidneys aren’t doing their job properly. They can’t get rid of phosphorus effectively or activate vitamin D. So, calcium levels drop and bam! The parathyroid glands kick into high gear.
When these glands overproduce PTH, calcium and phosphorus are released from your bones into the bloodstream to try to balance things out. But…too much PTH for a long time isn’t great either. It can lead to weakened bones—think of it as your skeleton saying “Hey buddy, we need a break!” This can make you more susceptible to fractures and other issues.
Now onto diagnosis. To figure out if someone has secondary hyperparathyroidism, doctors often look at blood tests measuring PTH levels along with calcium and phosphate levels. If those calcium numbers are low but PTH is high? Yeah, that’s a sign that something’s off in terms of how well the body handles these minerals.
Anyway, sometimes they might do imaging tests too—like ultrasounds—to check on those pesky parathyroid glands and see if they’re enlarged or up to no good. Those scans can really help paint a clearer picture.
When it comes to treatment options, there are several strategies depending on what’s causing this whole situation in the first place:
- Dietary changes: Increasing dietary calcium might help if that’s an issue.
- Vitamin D supplements: Getting vitamin D sorted is crucial since it helps increase calcium absorption.
- Phosphate binders: These are often used in patients with kidney issues to manage high phosphate levels.
- Surgery: In some cases where things get really out of hand—or if they’re dealing with complications—surgery may be necessary to remove some of the parathyroid tissue.
The thing is, managing secondary hyperparathyroidism isn’t just about throwing meds at a problem; it includes lifestyle changes too! Sometimes adjusting what you eat or getting more sunlight for vitamin D can have a massive impact.
So yeah, understanding this whole endocrine science thing is crucial because it helps us recognize how interconnected our body’s systems are. If one part isn’t functioning right—like our kidneys or our diet—it can end up affecting other areas significantly. And believe me when I say that keeping everything balanced is key!
Understanding Tertiary Hyperparathyroidism: Mechanisms, Diagnosis, and Management in Endocrinology
Sure! So, let’s talk about tertiary hyperparathyroidism. It’s like a twist in the body’s hormonal saga, and understanding it can feel a bit like piecing together a puzzle. You know what I mean?
Tertiary hyperparathyroidism usually occurs after an extended period of primary hyperparathyroidism or chronic kidney disease. Imagine if your parathyroid glands—those tiny little buddies located behind your thyroid gland—get overworked and cranky due to low calcium levels in your blood. They keep pumping out parathyroid hormone (PTH) like there’s no tomorrow.
Why does this happen? Well, the body tries to maintain balance. When kidneys fail to do their job properly, calcium levels take a dive. In response, the parathyroid glands go into overdrive releasing PTH to pull calcium from bones and increase its absorption in the intestines. Eventually, they just can’t chill out anymore, even when blood calcium levels normalize after treatment.
Now let’s chat about diagnosis. If you’re suspected of having this condition, doctors will check:
- PTH levels: Elevated PTH is a major indicator.
- Calcium levels: Typically high or normal after prolonged elevation.
- Vitamin D levels: These can be low due to kidney issues.
Testing might include imaging studies too. Sometimes, doctors use ultrasound or CT scans to check for any enlargement of those pesky parathyroid glands since they can get bigger when they’re working overtime.
As for management, it requires a good game plan tailored for each individual. Here are some common approaches:
- Medical treatment: Doctors might prescribe medications that help manage calcium levels.
- Surgery: If someone has persistent symptoms or complications, removing one or more parathyroid glands could be necessary.
- Dietary changes: Sometimes adjusting dietary intake of calcium and vitamin D helps.
It’s kind of like trying to get everyone in your friend group to agree on dinner plans—it takes some effort!
Honestly, managing tertiary hyperparathyroidism isn’t just about numbers; it involves looking at the whole person. If someone feels exhausted and achy due to fluctuating calcium levels and high PTH production, finding the right approach is so important!
So there you have it: basically how tertiary hyperparathyroidism works from mechanisms through diagnosis all the way to management! It’s definitely not an easy ride, but with proper care and understanding, things can improve significantly over time. Just remember that these tiny glands play a huge role in keeping our bodies balanced!
The Role of Vitamin D in the Management and Pathophysiology of Primary Hyperparathyroidism
So, let’s chat about vitamin D and its role in something called primary hyperparathyroidism. You might be thinking, “What’s that all about?” Well, here’s the scoop.
Primary hyperparathyroidism is a condition where your parathyroid glands, which are tiny glands in your neck, go a bit haywire. They produce too much parathyroid hormone (PTH). This hormone controls how much calcium is in your blood and bones. Normally, PTH helps keep calcium levels steady, but when it’s overproduced, things can get messy.
Calcium is super important for many functions in the body like muscle contraction and nerve signaling. When there’s too much calcium due to high PTH levels, you could face issues like weakened bones or even kidney stones. I once met someone who was always tired and had terrible bone pain. Turns out, they were dealing with this condition and didn’t even know it!
Now here comes vitamin D into the picture. Vitamin D helps your body absorb calcium from the food you eat. It’s like the sidekick to calcium’s superhero role! If you have low levels of vitamin D, you might not absorb enough calcium even if it’s present in your diet.
- Vitamin D deficiency: Low levels were often found in patients with primary hyperparathyroidism.
- PTH production: The body sometimes produces more PTH when calcium levels are low due to insufficient vitamin D.
- Bone health: Adequate vitamin D helps maintain strong bones by ensuring proper calcium absorption.
This connection can create a bit of a vicious cycle: low vitamin D leads to low calcium levels, which then triggers more PTH production. This can worsen the symptoms of primary hyperparathyroidism or even lead to further complications.
You know what else? Some studies suggest that boosting vitamin D intake might actually help manage primary hyperparathyroidism! It may lower blood PTH levels and improve calcium absorption without increasing bone turnover. So essentially, getting enough vitamin D could help keep that pesky hormone at bay.
But it’s kind of tricky because every person’s situation is different; it’s best to work with a healthcare provider to figure out what vitamin D level is right for you if you’re dealing with this condition.
The bottom line is: while primary hyperparathyroidism has its challenges, understanding how vitamin D plays a role can help navigate through them better. Just imagine getting more sunlight or eating those yummy fatty fish like salmon! Small changes could lead to better management of this condition and improvement in quality of life.
If you’ve got questions about your own health or someone’s else’s health related to this topic? Don’t hesitate to reach out—because knowledge is power!
Alright, let’s chat about hyperparathyroidism. It might sound like a mouthful, but it’s really just about our parathyroid glands—those tiny, often overlooked little dudes hanging out behind your thyroid. So, these guys are responsible for managing calcium levels in your body. Now, if they go a bit haywire and start producing too much parathyroid hormone (PTH), that’s when we step into the world of hyperparathyroidism.
Imagine you’re at a party, but instead of just one DJ controlling the music vibe, suddenly all four of them decide to crank up the volume at once. That’s basically what happens here! Your blood calcium levels shoot up because PTH’s got that party going and brings in tons of calcium from your bones and kidneys.
So let’s talk about how this plays out in real life. You know that feeling when you’re just so thirsty you can’t get enough water? Kind of like after a long run or a hot day? Well, that’s one symptom folks with hyperparathyroidism often experience because their kidneys are trying to deal with all that extra calcium and pushing out more urine. It can lead to dehydration over time—not fun at all!
But there’s more. You ever had those moments when you feel weirdly tired or foggy-headed? High calcium levels can make you feel exactly like that! It messes with your brain a bit—confusion, fatigue; it’s like trying to function while wearing someone else’s glasses that are super smudged.
And then there are those pesky kidney stones. Man, if you’ve ever heard someone talk about having kidney stones… ouch! Increased calcium can lead to stones forming like unwanted party crashers at our DJ’s event—and trust me; nobody wants those guys around.
Now here’s where it gets even more interesting: this isn’t just about feeling bad for yourself; it has deeper implications too. Chronic high calcium levels can lead to issues with bones and even make them weaker over time since they’re “giving away” their calcium too freely no pun intended.
When doctors see signs of hyperparathyroidism—like elevated PTH levels or one of those symptoms—it often leads them down the road of exploring what may be causing it in the first place. Sometimes it’s tied to other conditions or tumors on the glands themselves. Figuring this out is crucial because treating the root cause can really change someone’s quality of life dramatically.
So yeah, hyperparathyroidism might seem like another one of those medical whatchamacallits that’s easy to overlook, but understanding what’s happening under the hood is super important—not just for doctors but for anyone interested in health! It’s pretty wild how something so small can have such a massive impact on everyday life!